Home > Health & Welfare
Employee Health & Welfare

The Archdiocese of Cincinnati Welfare Benefit Plan is a non-ERISA ‘church plan’ with Grandfathered status under the Affordable Care Act (ACA).
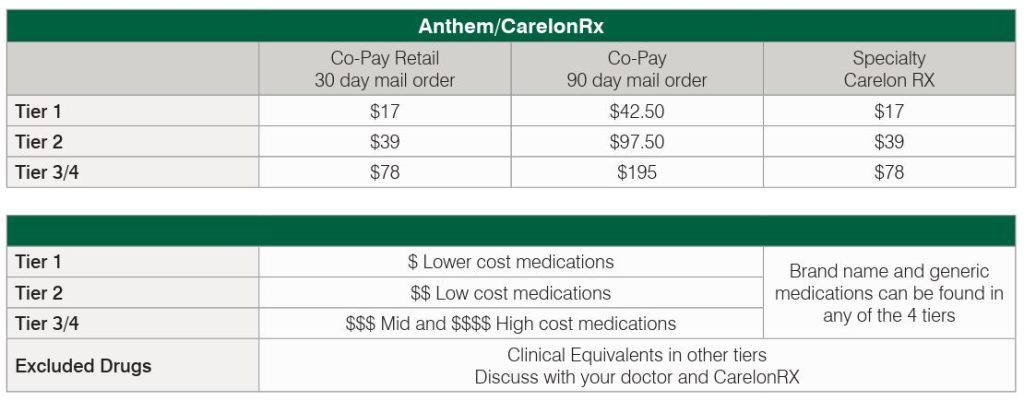
The administration of the medical & prescription drug program is processed through Anthem/CarelonRx.

The Archdiocese of Cincinnati Welfare Benefit Plan is a non-ERISA ‘church plan’ with Grandfathered status under the Affordable Care Act (ACA).
The administration of the medical & prescription drug program is processed through Anthem/CarelonRx.
Key information:
- You are able to access both your medical and pharmacy benefit information on the same platform via Anthem.com or the FREE Sidney Mobile App on a digital device.
- Your medical and pharmacy benefit are combined into one ID card under Anthem.
If you lose your Anthem/CarelonRx ID card, you can acquire a replacement by one of the following options:
- Download the Anthem Sydney App – have a digital ID card on a mobile device
- Register at Anthem.com – download/print or request copy to be mailed
- Call Anthem Customer Service at 1.833.727.2165
Anthem Family Advocate: Your Benefits Concierge
The Family Advocate is your first responder for everyday benefit questions. These concierge-level experts are hand-picked for their ability to find solutions quickly, helping you feel less overwhelmed.
They specialize in:
- Single-call support: Experts aim to resolve your health care needs in one conversation.
- Expert advocacy: Handling billing disputes and matching you with the right in-network providers.
- Expense reduction: Comparing hospital costs and accessing lower-cost generic medications.
- Health management: Getting help scheduling appointments and coordinating care between different specialists
Anthem Dedicated Clinical Advocates
When your health needs become more complex, a dedicated clinical advocate is provided who focuses on long-term clinical care and family support.
They provide:
- Expert care plans: In-house clinical experts help you create a personal wellness plan.
- Chronic care lead: Coordinates specialists and support for long-term health conditions.
- Personal advocates: Proactive support that anticipates your future health care needs.
- Rapid preapprovals: Speeds up the authorization process for urgent surgeries and medical care.
Anthem makes it easy to access both the Family Advocate & the Clinical Advocates by using a single point of entry.
Whether you have a quick billing question or a complex new diagnosis, you can reach your team the same way:
- Download the Anthem Sydney App – have a digital ID card on a mobile device
- Register at Anthem.com – download/print or request copy to be mailed
- Call Anthem Customer Service at 1.833.727.2165
Medical & Prescription Drug Plan Premium Rates
7/1/2025 – 6/30/2026
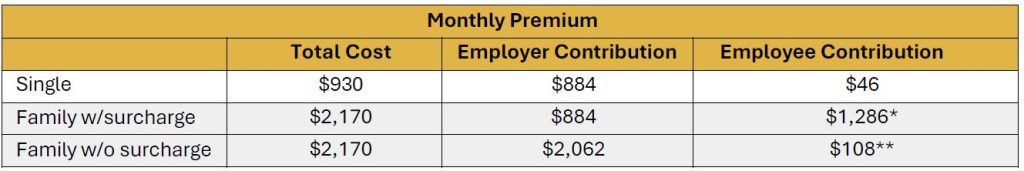
*The monthly family premium for employees whose spouse and/or dependents have access to other group health coverage is $1,286, which includes a $1,240 surcharge and a $46 single premium.
**The monthly surcharge can be waived when the employee provides evidence that their spouse and/or dependents do not have access to other group health coverage. Evidence is provided through an affidavit process.
The annual expense for a parish/school location is $10,608 for a single and $24,744 for a family plan for those employees who do not pay the surcharge.
The AOC Welfare Benefit Plan is a non-ERISA ‘church plan’ with Grandfathered status under the Affordable Care Act (ACA). Employees are offered single coverage with a low monthly premium. Family coverage is available to include the spouse and/or dependents with a monthly surcharge if the spouse and/or dependents have other group health plan coverage available to them. This monthly surcharge can be waived when the employee provides evidence that their spouse and/or dependents do not have access to other group health coverage. Employees are required to inform administration of any change in the availability of other group health coverage during the plan year as it may be considered a qualifying life event, potentially altering the waiver status of the surcharge for the remainder of the year.
Any false or misrepresented eligibility information will cause both your coverage and your dependents’ coverage to be retroactively terminated (to the extent permitted by law). Non-compliance is considered fraud and can result in recouping surcharge, claims paid and dismissal of those complicit in the fraud.
The Archdiocese of Cincinnati (AOC) Welfare Benefit Plan is a non-ERISA group health plan that maintains grandfather status under the Affordable Care Act (ACA). Employees are offered single coverage with a low employee premium charge. Family coverage is available to include the spouse and children, but with a monthly surcharge if the dependents have other group health plan coverage available to them. This monthly surcharge can be waived if it is determined the spouse and/or other parent is not eligible for other group health plan coverage.
The 2025-2026 plan year medical/prescription premium for single coverage is $930.00 per month. For eligible employees, the parish/school location pays $884.00 and the employee’s portion of the premium is $46.00 per month.
The 2025-2026 plan year medical/prescription premium for family coverage is $2,170.00 per month. For eligible employees, the parish/school location pays $2,062.00. The additional expense to a location for an employee’s family premium over the single premium is $1,240.00 per month. The employee may be subject to a monthly surcharge of $1,286.00 for this additional cost.
The surcharge can be waived when the employee provides evidence that their dependents have no access to other group healthcare coverage. Once the necessary steps to waive the surcharge are accomplished then the employee premium for family coverage is $108.00 per month.
Any change in the status of other available Group Health coverage during a plan year may be considered a Life Event and changes the waiver status for dependent surcharge during the plan year.
Any false or misrepresented eligibility information will cause both your coverage and your dependents’ coverage to be retroactively terminated (to the extent permitted by law). Non-compliance is considered fraud and can result in recouping surcharge, claims paid and dismissal of those complicit in the fraud.
Affidavit letters need to be downloaded by an employee requesting family coverage under the Archdiocese of Cincinnati Health Care Plan. The portion of the letter above the red line needs to be completed by that employee and then forwarded to the Human Resources Department of the employee’s spouse (and/or other parent of any dependent children) for completion. The employee requesting the family coverage under the Archdiocese of Cincinnati Health Care Plan returns the completed letter via email to: [email protected]. The Benefits Office will then process the completed letter for determination of surcharge waiver.
Sydney Health makes health care easier!
With just one click, you can:
- Find care and check costs
- See all benefits
- View Claims
- View and use digital ID cards
- Use the interactive chat feature to get answers quickly
- Sync your favorite fitness tracker
- Get started with Sydney Health – Follow this link to download the app
BOOST YOUR HEALTH…GET REWARDED
If you are enrolled in the AOC medical plan through Anthem – you are eligible to participate in the MyRewards program.
With MyRewards you can earn up to $300 each calendar year for participating in activities such as tracking your steps, completing a wellness exam, completing preventative services, and reading educational articles.
Start earning rewards through the Sydney App today. Download the no-cost Sydney Health app on your smart phone and;
- select Menu
- select Access Care
- select My Health Dashboard
- scroll down to My Rewards
Don’t have a smart phone – no problem you can also access MyRewards through Anthem.com:
- log in to anthem.com
- select My Health Dashboard
- select My Rewards
Note: Rewards earned must be redeemed before the end of the calendar year or you will lose them.
In need of orthopedic care – Hip, knee, spine or shoulder?
Partners in Health
The Archdiocese of Cincinnati has partnered with The Christ Hospital Joint and Spine Center to offer surgery benefits through the Center of Excellence program for hip & knee replacements, spine & shoulder procedures.
Members covered under the Archdiocese of Cincinnati health plan that utilize the Center of Excellence through the Christ Hospital for hip & knee replacement, spine & shoulder procedure are eligible to have the deductible and coinsurance waived for the procedure.
Tour the Christ Hospital Joint & Spine Center
Download an Informational Trifold
Call 513.557.4881 for spine care
Call 513.557.4882 for knee or hip replacement and shoulder procedures
Program Benefits Include:
Deductible and coinsurance waived for the procedure
Educational program prior to surgery
One number, one person who will coordinate scheduling the surgery, follow-up appointments and physical therapy
You will receive only one bill and explanation of benefits that includes:
- facility fees
- surgeon fees
- fees for other ancillary costs during the hospital stay


The Archdiocese of Cincinnati offers Hinge Health to employees and dependents 18+ enrolled in the Anthem plan.
Hinge Health is a digital exercise program that supports back and joint health. Hinge Health provides exercise therapy without leaving home and with no copays.
Hinge Health gives you the tools you need to conquer back and joint pain, recover from injuries, prepare for surgery, and stay healthy and pain free. Plus, you can complete your customized care plan anywhere, anytime.
Follow this link for more information: Archdiocese of Cincinnati and Hinge Health.
WHO IS ELIGIBLE FOR BENEFITS?
Active employees who are deemed eligible for benefits under the Archdiocese of Cincinnati Healthcare Plan, according to the plan provisions, must satisfy a waiting period prior to benefits becoming effective. Benefits will become effective the first day of the month following date of hire. This section of the Employee Benefits website is intended to be a summary of the eligibility provisions outlined in the Summary Document.
Eligibility for the Medical, Dental, Vision and FSA Plans
Full-time employees who work 30+ hours per week or teach 15+ classroom hours per week.Variable-hour employees who have worked an average of 30+ hours per week or have taught an average of 15+ classroom hours per week during the prior 12-month measurement period.Teachers who are employed by Athenaeum of Ohio and teach 14+ semester hours per year (or have taught an average of 14+ semester hours per year during the prior 12-month measurement period for variable hour teachers).
Eligibility for Life, AD&D and Long-Term Disability Insurance
All employees who are scheduled to work 20+ hours per week or teach 12+ classroom hours per week.Teachers who are employed by Athenaeum of Ohio and teach 9+ semester hours per year.
Applies to All Benefits
School employees are eligible if they meet the above-stated hourly requirements for the period of time school is in session.Employment at more than one location will be combined for eligibility purposes.
Eligible Spouses or Children
The plan allows coverage for your legal opposite-sex spouse and/or your child(ren) (biological, adopted, step or foster) from birth to the end of the month that your child attains age 26.Eligible spouses and dependent children may select the Archdiocese of Cincinnati Healthcare Plan even if the spouse has access to group medical insurance coverage as an employee or the child has access to group medical insurance coverage available through the employer of another parent. In this case, however, the Archdiocese will require the employee to pay 100% of the cost of the spouse or dependent coverage.
HOW DO I SELECT MY BENEFITS?
The Archdiocese of Cincinnati utilizes the online enrollment system, MyEnroll, for employee’s convenience to make selections for medical, prescription drug, flexible spending accounts, dental, life and long term disability insurance selections. MyEnroll is available online 24/7 for employees to review their Benefit record as well as monitor and submit FSA claims.
Enrollment choices and selections are available upon new hire and also during the annual open enrollment period. Consider your options carefully and follow the steps below to make smart enrollment choices.
Step 1: Confirm your eligibility and understand your options
Read through the 2025-2026 Enrollment Guide
Step 2: Plan for your needs
Review your current benefits and coverage levels: what make the most sense for you and your family?Decide which dependents you will cover; eligible employees have two coverage levels to choose from:Employee OnlyFamily
Step 3: Request your MyEnroll user ID and password
If you don’t already have a user ID and password, follow these steps to obtain one. The MyEnroll temporary issued password expires in 48 hours; if you do not log in within that time-frame, you will have to request another password.
Step 4: Gather proof documents for new dependents
Scan in necessary proof documents and save the documents to your desktop as one PDF per dependent. You will need to submit these during the online enrollment process by attaching the scanned documents to your MyEnroll file when promptedYou can also fax your proof documents to 1.887.265.2144
Step5: Enroll
Log onto MyEnroll using your user ID and password Click “Go” located within the pink box at the top of your MyEnroll pageWhen prompted, upload the necessary proof documents for new dependents. The proof documents can also be faxed to 1.887.265.2144.
Step 6: Conclude enrollment
Review the summary and signature page. If you are happy with your selections, click Accept and Finalize; this will conclude your enrolment.
WHAT ARE THE PROOF DOCUMENTS NEEDED TO ADD A DEPENDENT?
Legal Opposite-Sex Marriage
Marriage certificate (must be from local government)
Federal income tax return (first page – dollars may be redacted)
Biological Child
One of the following:
Birth certificate of biological child (listing Employee as parent)
Documentation on hospital letterhead indicating the birth date of child(ren) under 6 months old
Federal income tax return
Adopted Child
One of the following:
Official court/agency papers (initial stage)
Official Court Adoption Agreement (mid-stage)
Birth certificate (final stage)
Federal income tax return
Foster Child
Official court or agency placement papers
Stepchild
All of the following:
Child’s birth certificate showing the child’s parent is the employee’s spouse
Marriage certificate showing legal marriage between the employee and the child’s parent
Other Child
Court papers demonstrating legal guardianship, including the person named as legal guardian
Court-Ordered Medical Coverage
One of the following:
Qualified Medical Child Support Order (QMCSO
National Medical Support Notice (NMSN)
WHAT ARE QUALIFYING MID-YEAR LIFE EVENTS?
Employee contributions and FSA contributions are made on a pretax basis. Therefore, it is important that you make your elections during your enrollment period carefully because you can only make changes during the year if you have a qualifying mid-year life event according to IRS regulations listed below.
Changes to your Medical, Dental, Vision or Flexible Spending Account can be made if preceded by a documented qualifying life event and if they are made within 30 days of the event. Your change must be consistent with your life event/status change. The following events qualify for a change in coverage:
– Marriage
– Divorce or legal separation
– Birth or placement for adoption of a child
(When adding a new baby to the plan, call MyEnroll as soon as possible with the Social Security Number to ensure the baby’s coverage)
– Death of a dependent
– Ineligibility of a dependent
– Loss of other coverage
– Change in your employment status or that of your spouse
– Significant change in health coverage attributable to your employment or that of your spouse
– A court order
– Entitlement to Medicare or Medicaid
To make a change to your medical, dental or vision benefits or flexible spending account, you must experience a qualifying life event in accordance with IRS regulations.
If you experience one of these events and want to change your benefits, you must make the change within 30 days after the event occurs. Changes cannot be made before the event occurs. If you miss the window for making a change, there are no exceptions and you must wait to make an election during the next annual open enrollment period.
WHAT ARE THE PROOF DOCUMENTS NEEDED FOR A MID YEAR LIFE EVENT?
Mid-Year Life Event to remove a dependent:
Documentation (letter from new employer or new insurance carrier) showing coverage gained elsewhere including the date the coverage went into effect.
Mid-Year Life Event to add a dependent:
Documentation (letter from previous employer or previous insurance carrier) showing coverage lost, including the date the coverage terminate and those affected.
WHAT IS CONTINUATION OF COVERAGE?
As a church plan, the Archdiocese of Cincinnati’s Health Plan is not subject to federal COBRA coverage. The Plan is subject to Ohio’s continuation coverage requirements. The Archdiocese of Cincinnati offers continuation coverage to employees and their covered dependents who lose coverage under the Plan as a result of their involuntary termination of employment. To be eligible, you must have been covered by the Plan at the time of your termination of employment and your termination must not have been on account of gross misconduct. Contact your Business Manager or the Benefits Office at the Pastoral Center for the Archdiocese of Cincinnati for additional details.
WELFARE BENEFIT PLAN SUMMARY
This document is a summary of the Archdiocese of Cincinnati Welfare Benefit Plan (the “Plan”). This Plan includes the following benefits: (i) major medical and prescription drug plan (“Health Plan”), dental plan (“Dental Plan”), vision plan (“Vision Plan”), a health care flexible spending account (“Health FSA”), a dependent care flexible spending account (“Dependent Care FSA”), group life insurance coverage (“Group Life”), supplemental life insurance coverage (“Supplemental Life”), accidental death and dismemberment insurance (“AD&D”), and long-term disability benefits (“LTD”). Each of the welfare benefit plans described in this summary is intended to be a “church plan” as defined under §414(e) of the Internal Revenue Code and §3(33) of the Employee Retirement Income Security Act of 1974, as amended (“ERISA”) which has not made an election under §410(d) of the Internal Revenue Code to become subject to ERISA, and as such, is exempt from the requirements of ERISA.
Follow this link to review and/or download a copy of the Welfare Benefit Plan Summary.
SUMMARY OF BENEFITS AND COVERAGE (SBC)
The Summary of Benefits and Coverage document helps you chose a health plan. The SBC shows you how you and the plan share the cost for covered health care services. NOTE: Information about the cost of this plan (called the premium) is provided separately.
Follow this link to review and/or download a copy of the Summary of Benefits and Coverage (SBC).
CREDITABLE COVERAGE NOTICE
The Archdiocese of Cincinnati Health Plan has determined that the prescription drug coverage offered by Anthem/CarelonRx is, on average for all plan participants, expected to pay out as much as standard Medicare prescription drug coverage pays and therefore considered Creditable Coverage.
Download the Certificate of Creditable Coverage for Prescription Drug Notice.
PUBLICLY AVAILABLE COST INFORMAT/TRANSPARENCY IN COVERAGE
The link below leads to the machine readable files that are made available in response to the federal Transparency in Coverage Rule and includes negotiated service rates and out-of-network allowed amounts between health plans and healthcare providers. The machine-readable files are formatted to allow researchers, regulators, and application developers to more easily access and analyze data.
Click here – machine-readable-files
NOTICE OF PRIVACY PRACTICES
The Health Insurance Portability and Accountability Act of 1996 (HIPAA) requires the Archdiocese of Cincinnati Healthcare Plan, including each of its component health plans, (collectively the “Plan”) to provide you with this Notice that explains our privacy practices and outlines your rights under the Plan.
Click on this link to read, download or print the Privacy Practices Notice.
NOTICE OF NON-DISCRIMINATION
The Archdiocese of Cincinnati Healthcare Plan (the “Plan”) complies with applicable Federal civil rights laws and does not discriminate on the basis of race, color, national origin, age, disability, or sex. The Plan does not exclude people or treat them differently because of race, color, national origin, age, disability, or sex.
The Plan provides free aids and services to people with disabilities to communicate effectively with us, such as qualified sign language interpreters and written information in other formats (large print, audio, accessible electronic formats, other formats). Archdiocese provides free language services to people whose primary language is not English, such as qualified interpreters and information written in other languages. If you need these services, contact the Director of Human Resources of the Archdiocese at 513-263-6611
If you believe that the Plan has failed to provide these services or discriminated in another way on the basis of race, color, national origin, age, disability, or sex, you can file a grievance with: Rob Reid, Archdiocese of Cincinnati, Director of Human Resources, 100 E. Eighth Street, Cincinnati, OH 45202, Phone: 513-263-6611, Fax: 513-421-6225, Email: [email protected]. You can file a grievance in person or by mail, fax, or email.
You can also file a civil rights complaint with the U.S. Department of Health and Human Services, Office for Civil Rights, electronically through the Office for Civil Rights Complaint Portal, available at https://ocrportal.hhs.gov/ocr/portal/lobby.jsf, or by mail or phone at:
U.S. Department of Health and Human Services
200 Independence Avenue, SW
Room 509F, HHH Building
Washington, D.C. 20201
1-800-368-1019, 800-537-7697 (TDD)
Complaint forms are available at http://www.hhs.gov/ocr/office/file/index.html.
ATENCIÓN: si habla español, tiene a su disposición servicios gratuitos de asistencia lingüística. Llame al 513-421-3131.
注意:如果您使用繁體中文,您可以免費獲得語言援助服務。請致電 513-421-3131.
ACHTUNG: Wenn Sie Deutsch sprechen, stehen Ihnen kostenlos sprachliche Hilfsdienstleistungen zur Verfügung. Rufnummer: 513-421-3131
ملحوظة: إذا كنت تتحدث اذكر اللغة، فإن خدمات المساعدة اللغوية تتوافر لك بالمجان. اتصل برقم 513-421-3131
Wann du [Deitsch (Pennsylvania German / Dutch)] schwetzscht, kannscht du mitaus Koschte ebber gricke, ass dihr helft mit die englisch Schprooch. Ruf selli Nummer uff: Call 513-421-3131
ВНИМАНИЕ: Если вы говорите на русском языке, то вам доступны бесплатные услуги перевода. Звоните 513-421-3131.
ATTENTION : Si vous parlez français, des services d’aide linguistique vous sont proposés gratuitement. Appelez le 513-421-3131.
CHÚ Ý: Nếu bạn nói Tiếng Việt, có các dịch vụ hỗ trợ ngôn ngữ miễn phí dành cho bạn. Gọi số
XIYYEEFFANNAA: Afaan dubbattu Oroomiffa, tajaajila gargaarsa afaanii, kanfaltiidhaan ala, ni argama. Bilbilaa 513-421-3131.
XIYYEEFFANNAA: Afaan dubbattu Oroomiffa, tajaajila gargaarsa afaanii, kanfaltiidhaan ala, ni argama. Bilbilaa 513-421-3131.
주의: 한국어를 사용하시는 경우, 언어 지원 서비스를 무료로 이용하실 수 있습니다. 513-421-3131
ATTENZIONE: In caso la lingua parlata sia l’italiano, sono disponibili servizi di assistenza linguistica gratuiti. Chiamare il numero 513-421-3131.
注意事項:日本語を話される場合、無料の言語支援をご利用いただけます。513-421-3131
AANDACHT: Als u nederlands spreekt, kunt u gratis gebruikmaken van de taalkundige diensten. Bel 513-421-3131.
УВАГА! Якщо ви розмовляєте українською мовою, ви можете звернутися до безкоштовної служби мовної підтримки. Телефонуйте за номером 513-421-3131.
ATENȚIE: Dacă vorbiți limba română, vă stau la dispoziție servicii de asistență lingvistică, gratuit. Sunați la 513-421-3131.
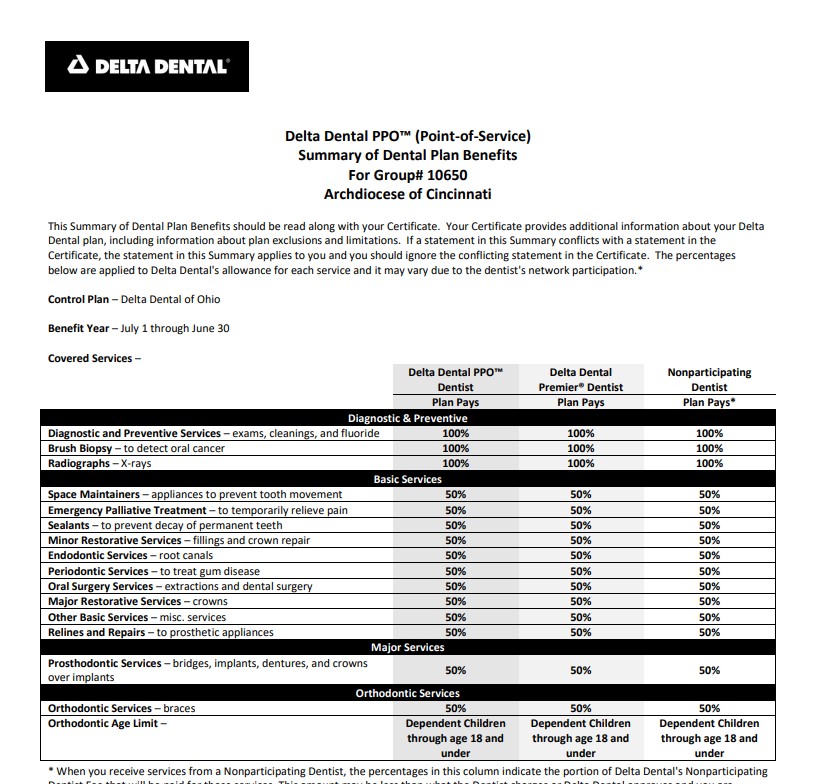
The Delta Dental of Ohio coverage for Archdiocese of Cincinnati enrolled members allows access to dentists in both the Delta Dental PPO & Delta Dental Premier networks at all times.
Members can bounce back and forth between the two networks (for example children can see a Premier pediatric dentist but also use a PPO orthodontist).
Benefit Year runs from July 1st through June 30th
Monthly Employee Cost
Single Coverage = $28.78
Family Coverage = $83.28
Delta Dental of Ohio issues ID cards in the name of the employee only…they do not provide an ID card to each covered family member.
Search the Delta Dental of Ohio website: www.deltadentaloh.com
Direct questions to Delta Dental of Ohio at 800.524.0149


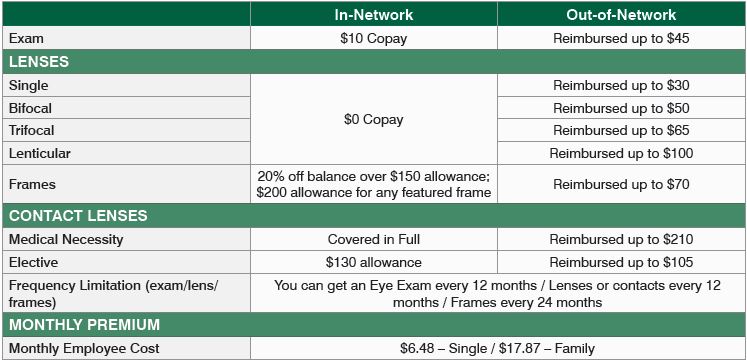
VSP does not issue ID cards. There’s no ID card necessary – just tell your eyecare provider you have VSP Vision coverage.
Search the VSP Vision website: www.vsp.com
Direct questions to VSP Vision at 800.877.7195
A flexible spending program allows an employee to commit a certain tax-free amount to a spending account set aside for healthcare and childcare expenses.
Reimbursements for allowable expenses within the Archdiocese of Cincinnati Healthcare Plan (dictated by Section 125 of the Internal Revenue Code) such as deductibles, copays, vision/dental expenses, childcare expenses.
Claims are submitted by the employee to MyEnroll by filling out necessary forms and providing required substantiation (receipts, invoices, etc.). Employees may also use the FSA debit card to pay for eligible healthcare expenses. The IRS requires that all FSA debit card transactions must be verified as eligible FSA expenses. Some transactions, such as standard copays, can be auto substantiated.
Still, many transactions require submission of supporting documentation to be verified. Multiple notifications from WEX Health will be sent to employees asking for substantiation. These notifications will be provided via email if an email address is available and will be sent from WEX Health. If an email address is not available, notifications will be mailed to the employee’s home. Upon final notice the FSA debit card will be frozen until substantiation is received.
A Dependent Day Care Flexible Spending Account (DFSA) allows you to set aside a portion of your salary, before tax, to reimburse certain amounts spent for eligible dependent day care expenses that are necessary in order for you, and if you are married, your spouse, to work or look for work.
What are the Claim Dates for Plan Year 2025?
Health Care FSA:
- Last Date to Incur Claims for Plan Year 2025 is 6/30/2026
- Last Date to Submit Claims for Plan Year 2025 is 9/30/2026
Dependent Day Care FSA
- Last Date to Incur Claims for Plan Year 2025 is 6/30/2026
- Last Date to Submit Claims for Plan Year 2025 is 9/30/2026
How much money can I contribute to my FSA?
Healthcare:
- Annual Maximum Contribution for the 2025-2026 Plan Year is $3,300 (minimum is $240)
- Carryover amount = $660.00
Dependent Day Care:
- Annual Maximum Contribution = $5,000 per couple for married filing jointly and single head of household
or
- $2,500 per individual for married filing separately (there is no minimum for dependent care)
What happens to my FSA if employment ends?
Should your employment terminate, your FSA participation will end on your last day of employment. Per the Internal Revenue Code, any funds remaining in your account, against which claims have not been incurred by or prior to your date of termination, will be forfeited.
What is a FSA debit card?
The FSA debit card is a special-purpose card that gives you an easy, automatic way to pay for qualified health care expenses that are eligible to be reimbursed through your Health Care FSA. The FSA debit card lets you access the pre-tax dollars you set aside in your FSA and use those dollars to pay for your eligible, reimbursable expenses.
I lost my FSA debit card – who do I contact for a replacement?
MyEnroll/Benefit Allocation Systems administers the Flexible Spending Account program for the Archdiocese of Cincinnati HealthCare Plan. Contact their Customer Service Team at 866.694.6423 or [email protected]
How does the FSA debit card change how I am reimbursed for FSA expenses?
With the FSA debit card, you simply swipe the Card and the funds are automatically deducted from your FSA. You must retain your receipts (provider receipts, not just credit card receipts) for all of your FSA debit card purchases. The benefit of the FSA debit card is that it eliminates most out-of-pocket cash outlays and you do not have to wait to receive reimbursement checks.
Why should I save receipts and other documentation for all purchases made with the FSA debit card?
The IRS requires that every transaction made with any type of Flexible Spending Account prepaid debit card, must be substantiated in order to confirm that the cardholder is using the Card to pay for an eligible FSA expense. The IRS considers many expenses paid with the FSA debit card to be automatically substantiated at the point of sale. For example, if you use your FSA debit card to pay a copayment amount for a prescription, the expense may be automatically substantiated if your plan’s copay amount is identified in the FSA debit card system. In this instance you do not have to separately submit a receipt for the copayment amount for substantiation. Many expenses cannot be substantiated at the point of sale, and IRS regulations require cardholders to submit supporting documentation in order to verify the transaction. Examples of expenses that may not automatically substantiate include dental, chiropractor and physician office visits where the amount paid is not equal to an established copay amount that is recognized in the FSA debit card system, and situations in which you charge more than on copay expense in the same FSA card swipe. If you use your FSA debit card for an expense that cannot be automatically substantiated at the point of sale, the merchant will be paid for the expense, but you MUST provide documentation to verify that the purchase is an appropriate FSA expense.
You will be required to submit substantiation to Benefit Allocation Systems, Inc. (“BAS”) in order to validate the eligibility of the expense in accordance with IRS guidelines.
What is the appropriate substantiation?
The Internal Revenue Service imposes certain rules on FSA contributions and distributions as a condition of allowing participants to receive the tax-favored benefits of FSA participation. One of those restrictions is that all FSA claims must be substantiated with supporting documentation that meets certain requirements. Appropriate substantiation includes the merchant or provider name, the service received or the item purchased the date, and the amount of the purchase.
Explanation of Benefits (EOBs) and other provider documentation may also be used as verification of an expense. Cancelled checks, handwritten descriptions of charges, card transaction receipts or previous balance receipts cannot be used to verify an expense.
Medical Service – An itemized receipt/statement or an EOB from the insurance company or health care provider should include: Patient Name; Provider Name; Date of Service; Description of Service (or procedure code); Amount Paid. A Credit Card receipt from your FSA debit card swipe is not sufficient.
Medical Item – Examples of a medical item include: nonprescription reading glasses, bandages for a current wound, contact lens solution, etc. A proper receipt should include: Merchant Name; Date of Purchase; Description of Item; Amount Paid. A Credit Card receipt from your FSA debit card swipe is not sufficient.
Prescription – Documentation for a prescription should include: Name of Patient; Name of Pharmacy; Date (fill date); Prescription Number or Name; Amount Paid. A Credit Card receipt from your FSA debit card swipe is not sufficient.
How long do I need to save my receipts and other documentation?
You should save all of your receipts and other documentation for as long as you would save documentation for your tax return. Consider keeping all information in one place so it is readily available upon request.
What if I lose my receipts or I accidentally swipe the Card for something that’s not eligible?
Usually, the service provider can recreate an account history and provide replacement documentation. Insurers can generally issue a replacement EOB. In the event that documentation cannot be located, recreated, or if the expense is ineligible for reimbursement, you can send a check or money order to BAS for the ineligible amount so BAS can forward the repayment to your employer for it to be credited back to your FSA. If this applies to you, please call BAS, 866.694.6423, for more information.
How will I know to submit documentation to verify a charge?
If there is a need to submit a receipt or other documentation, you will receive an email from WEX Health. The email will include an attachment with more information. Please DO NOT ignore emails you receive from Wex Health. You must respond to the emails from WEX Health in order to complete the process for documenting unsubstantiated expenses paid with your FSA debit card, as per the Card use agreement you received when you activated the Card. If you do not have an email associated with your account, you will receive the notifications through regular mail.
The majority of notifications will be sent each month for services rendered the prior month. However, ALL receipts should be saved per the IRS regulations as there may be instances in which you may have to submit documentation outside of the monthly notification.
What if I fail to submit documentation to verify a charge?
If you do not submit documents to verify an unsubstantiated charge made with the FSA debit card, then the Card will be suspended until proper documentation is received and the charge is substantiated. If it cannot be substantiated, you will be required to repay to your FSA the amount charged. BAS will advise you that your FSA debit card has been suspended if the documentation is not received when required. Submitting the appropriate documentation or repaying the amount in question will allow the FSA debit card to be reactivated.
What is the documentation request processing schedule for unsubstantiated claims?
If you use your FSA debit card for an expense that cannot be automatically substantiated, you will be asked for more information as follows:
- WEX Health will send you a letter requesting supporting documentation for the expense. If you have a valid email address entered into MyEnroll, you will receive the letter by email. you do not have an email address associated with your account, the letter will be mailed to your home address.
- You will have 30 days to respond to the first request for documentation. If your response is not received within 30 days, WEX Health will send you a second letter to remind you of the outstanding request for supporting documentation. If your response is not received within 30 days of your second notification (a maximum of 60 days from the first request), your FSA debit card will be suspended and you will receive a final notification asking for supporting documentation. Please note that you may continue to submit manual (paper or online) claims while the card is suspended.
- Your card will remain suspended until you provide adequate documentation, or until you repay your account with after-tax dollars. If you provide additional documentation, that documentation will be reviewed to determine if the expense can be properly paid from your FSA. If it is determined that the expense can be properly paid from your FSA, the claim will be substantiated and your FSA debit card will be reactivated. If after review of the documentation you submit, it is determined that there is not sufficient information to substantiate the claim, you will be sent another notification requesting more information. You will have 14 days to respond to the request for more information.
- If, based on all of the information you provide, it is determined that the expense is not an eligible expense, you will receive a notice asking you to send a check in the amount of the expense to reimburse your FSA. When BAS receives the repayment and your FSA is reimbursed for the ineligible expense, your account will be credited and your FSA debit card will be reactivated.
If you do not respond to the WEX health notifications within the identified timeframes, or if you do not repay an expense that is determined to be an ineligible expense, your FSA debit card may be permanently suspended and will not be reactivated.
Benefit Allocation Systems (BAS)/MyEnroll administers the Flexible Spending Account program for the Archdiocese of Cincinnati.
Direct questions to the customer services team: email: [email protected] or telephone 866.694.6423
The Archdiocese of Cincinnati provides eligible employees with $50,000 of Group Life and Accidental Death and Dismemberment (AD&D) insurance. Features of the Life coverage include a Right to Convert Provision, a Portability of Insurance Provision, Waiver of Premium (which will continue Life coverage without payment of premium while you are Totally Disabled), an Accelerated Benefit for the terminally ill and Travel Assist.
The Archdiocese of Cincinnati recognizes that different individuals have varying comfort levels and needs in regard to life insurance. It is important that you analyze a variety of factors to determine where you and your family need expanded coverage (e.g., risk factors, age, wellness, and medical history).
Benefit
- Remember that the Archdiocese of Cincinnati provides you with $50,000 coverage. For additional Group Term Life above the $50,000, employees can elect Supplemental Life Insurance in increments of $10,000 up to $500,000.
- The Employee must elect Supplemental Life coverage, in order for him/herself to elect coverage for a spouse/dependent. Spouse coverage amount can be elected in increments of $10,000, not to exceed the employee’s benefit amount.
- Eligible children may be covered from birth through age 26. You can elect a benefit amount of $2,500, $5,000, $7,500, or $10,000.
- If an employee or spouse elects or increases coverage during annual enrollment, an Evidence of Insurability* form must be completed and approved by The Standard (this form is available within the MyEnroll system).
- If an employee or spouse currently has the maximum Guaranteed Issue amount with The Standard at annual enrollment, they can apply for additional amounts of coverage; however, Evidence of Insurability* will be required.
*Benefit won’t become effective until Evidence of Insurability is approved by The Standard.
Long Term Disability (LTD) insurance provides income replacement in the amount of 60 percent of the first $8,333 of monthly pre-disability earnings, reduced by deductible income (e.g., work earnings, workers’ compensation, state disability, pension, etc.). The maximum monthly benefit is $5,000 and the minimum monthly benefit is $100. Benefits begin after a benefit waiting period of 180 days.
To be eligible for LTD insurance, for the benefit waiting period and the first 24 months for which LTD benefits are paid, you must be unable, as a result of physical disease, injury, pregnancy or mental disorder, to perform with reasonable continuity the material duties of your own occupation and suffering a loss of at least 20 percent of pre-disability earnings when working in the employee’s own occupation. After that, you must be unable as a result of physical disease, injury, pregnancy or mental disorder to perform with reasonable continuity the material duties of any reasonable gainful occupation. You are not considered disabled when earning 80 percent or more of pre-disability earnings in any occupation.
An eligible employee who needs to make a Long-Term Disability claim can do so by notifying his/her Location Administrator, who will help facilitate the process. LTD claims must be approved by The Standard Insurance Company.
Direct questions to The Standard Insurance Company member services at: 800.628.8600

An EAP is a free service that provides access to counselors and resources to help employees and their household members with everyday problems and questions.
How do I access the EAP?
You can access the EAP 24 hours a day either online or via phone, and there is never any need to make an appointment first.
Online, you have access to articles, checklists, webinars, online classes and other helpful tools. Navigate to www.anthemeap.com/aoc.
Via phone, 800.865.1044, EAP counselors are able to assist with setting up one of your four (4) free counseling sessions* with a licensed professional. They are also able to direct you to professionals and experts able to consult with you on various topics.
The Archdiocese of Cincinnati 401(k) Plan became effective January 1, 2011. This Plan is an important benefit intended to help employees in their retirement years as a supplement to their personal retirement savings, Social Security benefits, the frozen Archdiocese of Cincinnati Pension Plan for Lay Employees and the terminated Archdiocese of Cincinnati 403(b) Plan.
Eligible participants can: (1) make their 401(k) elective contributions; (2) receive Archdiocese base contributions; and (3) receive favorable tax advantages through either traditional or Roth 401(k) elections.
Specific 401(k) account details, investment options, and additional retirement readiness tools are attainable through the Empower Retirement participant website – empowermyretirement.com
Accessing and Managing Your Account
The Plan offers flexible account access options that help you stay connected, manage your account, and make the most of your plan benefit so you can look to the future with confidence.
- Website: empowermyretirement.com
- Mobile App: Empower Retirement
- Empower Retirement Participant Services Line: 1-866-467-7756
- Retirement Representatives: weekdays 8:00 am -10:00 pm ET and Saturdays 9:00 am – 5:30 pm ET
Beneficiary Designation
Ensure your retirement assets end up in the hands of those intended.
Keep your beneficiary information up to date:
Log on to your account via empowermyretirment.com and follow these easy steps:
1. Go to > Accounts
2. Select > Beneficiaries
Empower Education Series
Join Empower during the month of March for a live webinar: Maximize Your Savings with an Experience Built Around You
- A look at your savings
- Saving in your plan
- Resources designed for you
Join Empower throughout 2026 for their live webinars. Topics available through this link.
Register for any session at: www.learningfromempower.com
The Lay Employees of the Archdiocese of Cincinnati Pension Plan was frozen on December 31, 2010.
The Plan provides a monthly pension benefit at retirement, for vested employees hired prior to December 31, 2010.
An employee must be vested in the Plan to be entitled to a benefit. To commence retirement benefit payments, apply to UMR, the Contract Administrator for the Plan by calling 888.640.1700
Termination of the Archdiocese of Cincinnati 403(b) Plan
The Archdiocese of Cincinnati 403(b) Plan was “frozen” effective December 31, 2010, and no further contributions could be made to the 403(b) Plan.
This 403(b) Plan was formally terminated effective December 31, 2015. Lay-employee participants in the Archdiocese of Cincinnati 403(b) plan have a “distributable event” on account of its termination and should contact their 403(b) Plan vendor to elect a distribution.
As you begin to plan for retirement below are considerations to keep in mind:
There is no application form to be completed to retire from a location within the Archdiocese of Cincinnati. It is not necessary to notify the Pastoral Center at the Archdiocese of your upcoming retirement, however, the Benefits Office is available to answer questions when you are navigating through the process. Learn more by downloading an FAQ informational flyer.
- Be sure to touch base with your Parish/School/Agency business manager so they are aware of your intent to retire.
If your employment occurred prior to December 31, 2010 you might be vested in the frozen Lay Employees defined pension plan. Contact UMR, Administrator of the Lay Employees Pension Plan at 1.888.640.1700.
If you are an eligible participant in the Archdiocese of Cincinnati 401(k) plan contact the Customer Care team at empowermyretirement.com, 866.467.7756, for information on rollover and/or withdrawal options.
Effective December 31, 2016, the Archdiocese of Cincinnati terminated its Supplemental Retiree Health Insurance Plan and Retiree Dental Plan for Post-65 lay retirees. Effective September 1, 2016, the Pre-65 Retiree Health Plan and Pre-65 Retiree Dental Plan were frozen and no longer accept any new participants.
All Archdiocese of Cincinnati lay employees, retirees, and their spouses can benefit from the RetireMed program. RetireMed is a completely free resource that provides expert guidance as you transition from employer health coverage to Medicare or Marketplace plans. Their team of licensed advisors is dedicated to making this process simple, stress-free, and tailored to your unique needs. What sets RetireMed apart is their lifelong support—once you enroll, their team remains available to answer questions, review your coverage annually, and help you navigate any changes in your health care needs. Whether you’re planning for retirement soon or just want to understand your options. Please follow the link by clicking here if you’d like more information or to schedule a consultation.
If you haven’t already done so it is important to begin the process of applying for Medicare Parts A & B. Follow this link for Medicare information.
The intent of these Employee Health & Welfare webpages is to provide general information regarding archdiocese resources and partner relationships. It does not necessarily fully address all specific issues. It should not be construed as, nor is it intended to provide, legal advice. The Archdiocese of Cincinnati Healthcare Plan fully complies with the ethical and religious directives of the United States Conference of Catholic Bishops. The Archdiocese of Cincinnati reserves the right, in its sole discretion, to amend, modify, or terminate the Plan at any time
These Employee Benefits webpages are an outline of the coverage and services provided by the carrier(s) or vendor(s). They do not include all of the terms, coverage, exclusions, limitations, and conditions of the actual contract language. The policies and contracts themselves must be read for those details and are available for your reference through Archdiocese of Cincinnati or upon request.
